EXCELLENTTrustindex verifies that the original source of the review is Google. I visited Physio- Soton multiple times now. I can only say, Marek and Piotr they both provide exceptional care. 5 stars well deserved.Posted onTrustindex verifies that the original source of the review is Google. Lovely environment Really knowledgeable about where to poke and prod, feeling much better and able to move again with out discomfort Looking forward to going againPosted onTrustindex verifies that the original source of the review is Google. I had an excellent experience with Marek. The clinic is equipped with advanced diagnostic tools, including ultrasound, which made the assessment very precise. Marek is highly experienced and exceptionally qualified, providing clear explanations and effective treatment plans. Professional, knowledgeable, and genuinely focused on patient care—highly recommended!Posted onTrustindex verifies that the original source of the review is Google. Thank you Marek. Very professional, knowledgeable and prompt with appointment regarding a recent shoulder injury. Appointment within 24 hours A significant tear in my shoulder tendon. Treatment begins straight away. Previous experience with the NHS on my other shoulder., a good 6 week wait for a scan. The sooner you begin treatment the better. The cost was very competitive and reasonable. Parking at the back of the practice, which is impeccably clean. Its the best £120 i have spent. Worth every penny Thank youPosted onTrustindex verifies that the original source of the review is Google. I had an ultrasound and consultation with Marek for a tennis elbow. He was super clear throughout and explained what he was seeing and showed me what the issue was. Very thorough discussion on various options and very transparent about the pros and cons of all of them. Great guy! Thanks!Posted onTrustindex verifies that the original source of the review is Google. Lee Saunders I had a knee problem and the service is 100% gives you great advice. Don’t rush treatment now my knee 100% better now. I’ve had an injection with recommend to anyone who’s got any injuries or muscle problems or joint problems first class servicePosted onTrustindex verifies that the original source of the review is Google. I visited Marek’s clinic yesterday for a knee scan because I had been experiencing pain for some time. I’m very satisfied with the professional care and attention I received. Marek was kind, thorough, and explained everything clearly. I highly recommend his clinic to anyone looking for excellent medical support.Posted onTrustindex verifies that the original source of the review is Google. Amazing service from Marek…. I called Marek and explained my situation regarding my shoulder pain , which I’ve suffered with over the years. Marek scanned my shoulder, diagnosed and educated me with the injury and then proceeded with the treatment. I found Marek very informative and professional, which in turn put me at ease. It was a relief to know what was causing my shoulder pain to flare up from time to time and Marek put in place a plan for shoulder injury going forward if it flares up again. Thank you for a top service !!!Posted onTrustindex verifies that the original source of the review is Google. I injured my shoulder at the gym couldn't lift my hand , I messaged Marek and next they they done scan ,we exactly know what happened, great clinic, can recommend on 100%Posted onTrustindex verifies that the original source of the review is Google. I cannot reccommend Physio soton enough, Marek put me at ease, listened and worked with me to cure my back pain. I would not hesitate to use them again!
This page is intended for educational purposes. If you would like to book an appointment or need support with shoulder bursitis, please get in touch with Physio Soton Clinic in Eastleigh, near Southampton.
Shoulder bursitis is a common condition that causes pain, stiffness, and limited movement in the shoulder joint. It occurs when the bursa—a small, fluid‑filled sac that cushions and reduces friction between tissues—becomes irritated or inflamed.
This page explains what shoulder bursitis is, why it happens, and how it’s commonly managed.
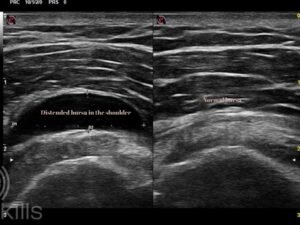
In the shoulder, the most commonly affected bursa is the subacromial bursa, which sits between the rotator cuff tendons and the bony part of the shoulder (the acromion). When this bursa becomes inflamed, normal shoulder movements can become painful and restricted.
Shoulder bursitis may develop on its own or alongside other shoulder problems such as rotator cuff tendinitis or impingement.
Symptoms can range from mild to severe and may include:
Dull, aching pain on the outer or front of the shoulder
Pain that worsens when lifting the arm or reaching overhead
Shoulder stiffness or reduced range of motion
Pain when lying on the affected shoulder
Tenderness or swelling around the shoulder joint
Symptoms may come on gradually or appear suddenly after overuse or injury.
Shoulder bursitis is often caused by repetitive stress or irritation. Common causes include:
Repetitive overhead movements (sports, work tasks, or daily activities)
Poor posture or shoulder mechanics
Sudden injury or trauma to the shoulder
Prolonged pressure on the shoulder
Muscle weakness or imbalance around the shoulder
Risk may be higher for people who:
Perform repetitive arm movements (e.g., painters, athletes)
Have poor posture or rounded shoulders
Are over the age of 40
Have underlying shoulder or neck conditions
Diagnosis is usually based on:
A review of symptoms and activity history
Physical examination of shoulder movement and strength
Imaging tests (such as ultrasound or MRI) if needed to rule out other conditions
While the subacromial bursa is the most commonly affected in shoulder bursitis, several other bursae around the shoulder can also become inflamed. The subdeltoid bursa, which sits beneath the deltoid muscle, is often involved alongside the subacromial bursa, and the two are frequently described together as the subacromial–subdeltoid bursa. Less commonly, the subcoracoid bursa at the front of the shoulder can cause anterior shoulder pain, particularly with forward lifting or rotation movements. The subscapular bursa, located deeper at the front of the joint, may also become irritated and can sometimes communicate with the shoulder joint itself. In rarer cases, inflammation of the scapulothoracic bursae, found between the shoulder blade and chest wall, can cause pain along the upper back and may be associated with a grinding or snapping sensation. However, in clinical practice, most cases of shoulder bursitis involve the subacromial–subdeltoid bursa.
Treatment typically focuses on reducing inflammation, relieving pain, and restoring movement.
Rest and activity modification to avoid aggravating movements
Ice or heat therapy to reduce pain and inflammation
Anti‑inflammatory medications, if appropriate
Physical therapy to improve strength, posture, and shoulder mechanics
Corticosteroid injections may be considered if symptoms persist
Advanced treatments or referral if conservative care is not effective
Most cases improve with non‑surgical treatment and proper rehabilitation.
Recovery time varies depending on severity and activity level. To help prevent recurrence:
Maintain good posture
Strengthen shoulder and upper back muscles
Warm up before physical activity
Avoid repetitive overhead strain when possible
Address shoulder pain early
You should seek medical or physiotherapy advice if:
Shoulder pain lasts more than a few weeks
Pain is severe or worsening
Movement becomes increasingly limited
Symptoms interfere with sleep or daily activities
Early assessment can help prevent long‑term shoulder problems.
Shoulder bursitis is a painful but often manageable condition. With appropriate care, activity modification, and rehabilitation, most people experience significant improvement and return to normal function.
If you are experiencing ongoing shoulder pain, a professional assessment can help determine the cause and guide effective treatment.
Q: What is shoulder bursitis?
A: Shoulder bursitis is inflammation of the shoulder’s bursa, most commonly the subacromial bursa. It causes pain, stiffness, and limited movement, especially when lifting the arm.
Q: What are the symptoms of shoulder bursitis?
A: Symptoms include outer or front shoulder pain, stiffness, tenderness, swelling, pain with overhead movements, and discomfort when lying on the affected side.
Q: How is shoulder bursitis treated?
A: Treatment includes rest, activity modification, ice or heat, anti-inflammatory medication, physiotherapy, and, if needed, corticosteroid injections into the subacromial bursa.
Q: Can shoulder bursitis heal on its own?
A: Mild cases may improve with rest, but most benefit from physiotherapy to prevent recurrence. Persistent pain should be assessed by a professional.
Q: How long does recovery take?
A: Mild shoulder bursitis can improve in a few weeks; moderate or chronic cases may take 6–12 weeks or longer with proper care and rehabilitation.
Q: When should I see a physiotherapist?
A: Seek assessment if pain lasts more than a few weeks, limits movement, or affects daily activities. Early treatment improves recovery and prevents long-term shoulder issues.
 Marek Czeladzki is a highly skilled physiotherapist, musculoskeletal (MSK) sonographer, independent prescriber, and injection therapist based in Southampton. He specialises in diagnosing and treating a wide range of musculoskeletal conditions, using advanced ultrasound imaging to accurately assess soft tissue and joint issues. As an independent prescriber, Marek can provide targeted medication when appropriate, and his expertise in therapeutic injections allows him to deliver effective, minimally invasive treatments for conditions such as shoulder bursitis, joint pain, and tendon injuries. Combining hands-on physiotherapy techniques with his advanced diagnostic and interventional skills, Marek provides personalised care aimed at reducing pain, improving function, and supporting long-term recovery.
Marek Czeladzki is a highly skilled physiotherapist, musculoskeletal (MSK) sonographer, independent prescriber, and injection therapist based in Southampton. He specialises in diagnosing and treating a wide range of musculoskeletal conditions, using advanced ultrasound imaging to accurately assess soft tissue and joint issues. As an independent prescriber, Marek can provide targeted medication when appropriate, and his expertise in therapeutic injections allows him to deliver effective, minimally invasive treatments for conditions such as shoulder bursitis, joint pain, and tendon injuries. Combining hands-on physiotherapy techniques with his advanced diagnostic and interventional skills, Marek provides personalised care aimed at reducing pain, improving function, and supporting long-term recovery.